Most health sensors today are built for adult patients. It’s a larger patient population than the pediatric patients who could benefit from sensors - but that doesn’t make sensors any less important for children’s healthcare.
It’s important to remember that children are not small adults, and we can’t simply re-size adult treatments for children. They have specific needs in childhood, particularly in the Neonatal Intensive Care Unit (NICU). Zansors, in collaboration with George Washington University, is working to create sensors for pediatric care with grant award (R41HD088142) from Eunice Kennedy Shriver National Institute of Child Health and Human and Development (NICHD). With funding from NICHD, Zansors will work to reduce the pain a baby feels from needle prick and reduce amount of blood collected.
Glucose monitoring is an area where sensors can change the way care is delivered in the NICU today. For many babies, high blood sugar accounts for illness or stress, but for those born prematurely, it’s much more common. This is because the pancreas, which makes insulin, is not fully developed.
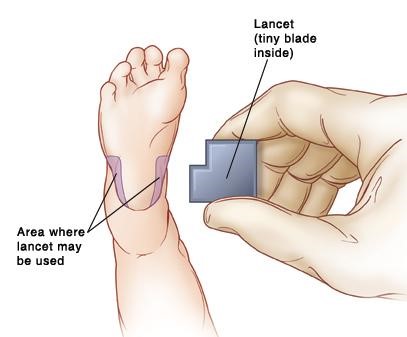
Today, we often monitor glucose in the NICU through a tiny blade, that takes a drop of blood from the baby’s foot. Then, this is used to measure glucose in a small test strip.
Source: Fairview Health System https://www.fairview.org/patient-education/88155
If a baby is in an at-risk group, blood glucose will be checked this way at two hours of age, and before the baby feeds, which can be three to five times over the first two days of their life.
Instead of testing every three hours, Zansors is working to monitor continuously through a sensor patch. This alternative continuous glucose monitoring is different because it’s monitoring constantly under the skin, instead of via occasional heel sticks. Not only is less blood drawn, but that blood is drawn less frequently, only once every 24 hours compared to several times throughout the day.
We already use continuous glucose monitoring for adults and children with diabetes, but research is still underway to support the same resolution for preterm infants. Studies show that continuous monitoring is reliable in the NICU, but we need more studies to establish it as the safest way to measure glucose.
Zansors is working to make sensors that can do this. It will reduce pain and help us alleviate stress caused to babies in the NICU by eliminating or reducing the number of heel sticks needed. In addition, if a baby’s glucose levels change, the medical care team will be alerted immediately, not just when testing takes place.
Watch our animation to see exactly how continuous glucose monitoring can make a difference:
Research reported in this publication was supported by the Eunice Kennedy Shriver National Institute Of Child Health & Human Development of the National Institutes of Health under Award Number R41HD088142. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.